Business Wire India
Masimo (NASDAQ: MASI) announced today the findings of a study recently published in BMC Anesthesiology in which researchers at University Hospital Linköping, Sweden, compared the performance of goal-directed fluid therapy (GDFT) using invasive esophageal Doppler to GDFT using Masimo PVi® (pleth variability index, measured noninvasively and continuously using SET® pulse oximetry sensors) in patients undergoing major abdominal surgery.1
This press release features multimedia. View the full release here: https://www.businesswire.com/news/home/20180904005977/en/
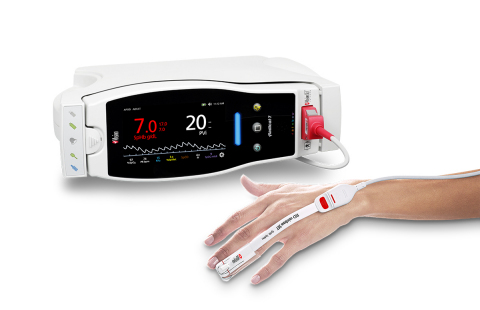
Masimo Radical-7® with PVi® (Photo: Business Wire)
Noting the value of GDFT in aiming to determine “the optimal amount of fluid for an individual patient,” Dr. Hans Bahlmann and colleagues sought to compare the effects of two methods of GDFT, stroke volume optimization guided by invasive esophageal Doppler (control group) and fluid optimization guided by noninvasive PVi (intervention group), on patients who were scheduled for open abdominal surgery lasting two or more hours. The effects compared were incidence of complications and length of hospital stay.
The researchers collected data from 146 patients who had surgery between November 2011 and January 2015, who were randomly divided into the two groups. In the intervention group, PVi was noninvasively and continuously measured with a Masimo Radical-7® Pulse CO-Oximeter® with software version 7.8.0.1 and SET® sensors. After an initial fluid bolus (given to all patients irrespective of PVi value), a fluid bolus was given if PVi was ≥ 10%, repeated at 5 minute intervals until PVi fell below 10% or did not decrease at all. In the control group, esophageal Doppler measurements were performed using a Deltex Medical CardioQ apparatus. After an initial fluid bolus, Doppler measurement was performed after 5 minutes and fluid boluses were repeated until stroke volume did not increase by 10%, in accordance with published protocols.
Observers blinded to each patient’s group assessed complications for 30 postoperative days using a pre-specified list of complications, as well as length of hospital stay. The researchers found that noninvasive PVi and invasive Doppler performed with no statistical difference, with similar incidences of complications and lengths of stay between the two groups. In the intervention/PVi group, there were 64 complications (corresponding to 51% of patients), with a median length of stay of 8.0 days (interquartile range [IQR] 8.0 days). In the control/Doppler group, there were 70 complications (corresponding to 49% of patients), with a median length of stay of 8.0 days (IQR 9.5).
The researchers concluded, “No difference in clinical outcome, as defined by number of postoperative complications, and length of hospital stay, was found when goal-directed fluid therapy was applied using PVi as an alternative to esophageal Doppler. PVi appears to be an acceptable alternative to esophageal Doppler for goal-directed fluid therapy during major open abdominal surgery.”
In discussing other PVi-related clinical studies, the researchers also noted that “Based on these reports and our findings, a clinician wishing to pursue GDFT can choose PVi over esophageal Doppler in the large majority of patients undergoing major open abdominal surgery. PVi, in contrast to esophageal Doppler, is not sensitive to interference from diathermy and does not require frequent access to the patient’s head for probe repositioning. Also, PVi can be measured without single-use equipment, avoiding the cost for single-use esophageal probes (USD 130 in our setting). However, as illustrated by the request for Doppler data in two PVi patients, the clinician might still want to have access to a reliable method for measuring intraoperative cardiac output to increase the amount of hemodynamic information during unusually complex situations or in cases of known vascular and/or myocardial dysfunction.”
As a study limitation, the researchers noted the absence of a control group with neither PVi nor Doppler guiding fluid therapy, and therefore “it is not possible to tell whether PVi and Doppler both result in similar improvements in outcome, or whether neither method improves outcome when compared to treatment without GDFT.” They also noted that because of determining sample size using a 10% difference in the number of complications at 30 days, “the study was not powered to detect smaller albeit still significant differences in postoperative outcome.”
PVi has not been cleared by the FDA to assess fluid responsiveness.
@MasimoInnovates | #Masimo
Reference
- Bahlmann H, Hahn R, and Nilsson L. Pleth variability index or stroke volume optimization during open abdominal surgery: a randomized controlled trial. BMC Anesthesiology. (2018) 18:115. https://doi.org/10.1186/s12871-018-0579-4.
About Masimo
Masimo (NASDAQ: MASI) is a global leader in innovative noninvasive monitoring technologies. Our mission is to improve patient outcomes and reduce the cost of care. In 1995, the company debuted Masimo SET® Measure-through Motion and Low Perfusion™ pulse oximetry, which has been shown in multiple studies to significantly reduce false alarms and accurately monitor for true alarms. Masimo SET® has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,1 improve CCHD screening in newborns,2 and, when used for continuous monitoring with Masimo Patient SafetyNet™ in post-surgical wards, reduce rapid response activations and costs.3,4,5 Masimo SET® is estimated to be used on more than 100 million patients in leading hospitals and other healthcare settings around the world,6 and is the primary pulse oximetry at 9 of the top 10 hospitals listed in the 2018-19 U.S. News and World Report Best Hospitals Honor Roll.7 In 2005, Masimo introduced rainbow® Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb®), oxygen content (SpOC™), carboxyhemoglobin (SpCO®), methemoglobin (SpMet®), Pleth Variability Index (PVi®), and more recently, Oxygen Reserve Index (ORi™), in addition to SpO2, pulse rate, and perfusion index (Pi). In 2014, Masimo introduced Root®, an intuitive patient monitoring and connectivity platform with the Masimo Open Connect® (MOC-9®) interface, enabling other companies to augment Root with new features and measurement capabilities. Masimo is also taking an active leadership role in mHealth with products such as the Radius-7® wearable patient monitor, iSpO2® pulse oximeter for smartphones, and the MightySat™ fingertip pulse oximeter. Additional information about Masimo and its products may be found at www.masimo.com. Published clinical studies on Masimo products can be found at http://www.masimo.com/evidence/featured-studies/feature/.
ORi has not received FDA 510(k) clearance and is not available for sale in the United States.
The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
- Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
- de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
- Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
- Taenzer AH et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
- McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
- Estimate: Masimo data on file.
- http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.
Forward-Looking Statements
This press release includes forward-looking statements as defined in Section 27A of the Securities Act of 1933 and Section 21E of the Securities Exchange Act of 1934, in connection with the Private Securities Litigation Reform Act of 1995. These forward-looking statements include, among others, statements regarding the potential effectiveness of Masimo PVi®. These forward-looking statements are based on current expectations about future events affecting us and are subject to risks and uncertainties, all of which are difficult to predict and many of which are beyond our control and could cause our actual results to differ materially and adversely from those expressed in our forward-looking statements as a result of various risk factors, including, but not limited to: risks related to our assumptions regarding the repeatability of clinical results; risks related to our belief that Masimo's unique noninvasive measurement technologies, including Masimo PVi, contribute to positive clinical outcomes and patient safety; risks related to our belief that Masimo noninvasive medical breakthroughs provide cost-effective solutions and unique advantages; as well as other factors discussed in the “Risk Factors” section of our most recent reports filed with the Securities and Exchange Commission (“SEC”), which may be obtained for free at the SEC's website at www.sec.gov. Although we believe that the expectations reflected in our forward-looking statements are reasonable, we do not know whether our expectations will prove correct. All forward-looking statements included in this press release are expressly qualified in their entirety by the foregoing cautionary statements. You are cautioned not to place undue reliance on these forward-looking statements, which speak only as of today's date. We do not undertake any obligation to update, amend or clarify these statements or the “Risk Factors” contained in our most recent reports filed with the SEC, whether as a result of new information, future events or otherwise, except as may be required under the applicable securities laws.
View source version on businesswire.com: https://www.businesswire.com/news/home/20180904005977/en/
![]()
MULTIMEDIA AVAILABLE :
https://www.businesswire.com/news/home/20180904005977/en/